"Super bacteria," namely infections that have mutated to become resistant to drugs due to the over-usage of antibiotics, kill over 50,000 people in the US and Europe and hundreds of thousands more world-wide every year. The answer to the problem may lie in an unlikely place - Jerusalem sewers.
Giving a sense of the scope of the danger, the Review on Antimicrobial Resistance commissioned by the UK found that if the problem is not addressed, by 2015 drug-resistant infections could cause 10 million deaths a year and cost up to $100 trillion.
But a pioneering research team led by Dr. Ronen Hazan of the Hebrew University of Jerusalem's Institute of Dental Sciences, as well as Dr. Nurit Beyth and a group of colleagues and students, may have found a breakthrough in confronting the danger.
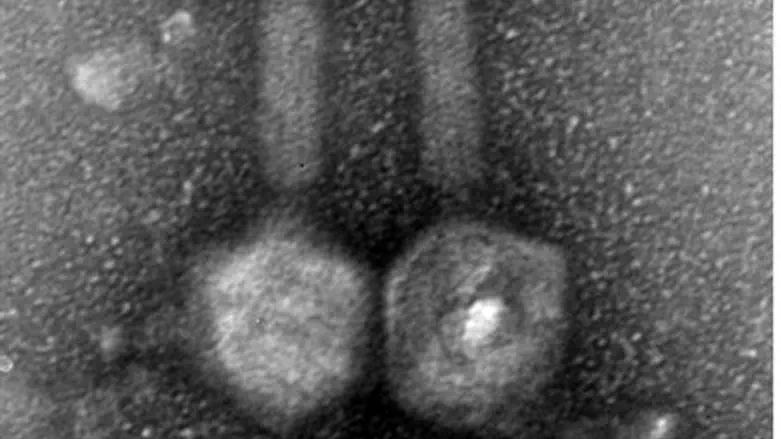
The team found that the way to defeat the mutating bacteria appears to be through bacterial warfare, infecting the harmful bacteria with tiny viruses called bacteriophages or "phages" that co-evolve with the bacteria they infect and become "professional bacterial killers."
A phage against Enterococcus faecalis, a life-threatening pathogen common in post-root canal infections, was isolated by the researches from sewage effluents gathered at a Jerusalem sewage treatment facility. The phage, called EFDG1, can infect E. faecalis which antiobiotics have failed to conquer.
EFDG1 was found to work in combating the bacteria, and succeeded both in vitro and ex vivo in tissue samples, suggesting the phage can stop infection following root canals.
But is the sewer-based bacteria safe for humans?
To find out the researchers investigated the phage with electron microsopy and whole genome sequencing, finding that it does not contain apparent harmful genes.
"The idea of using phages as anti-bacterial drugs is not new," said Dr. Hazan. "Phage therapy was first proposed at the start of the 20th century, but then abandoned for various reasons, including the striking success of chemical antibiotics."
Hazan continued "now we stand on the verge of a new era with the limitations of synthetic antibiotics and the emergence of antibiotic-resistant strains of bacteria. Thus it is the right time to look again into what Mother Nature offers in the battle against bacteria. As this research shows, bacteriophages may prove an effective tool in the development of much-needed new antimicrobial drugs."