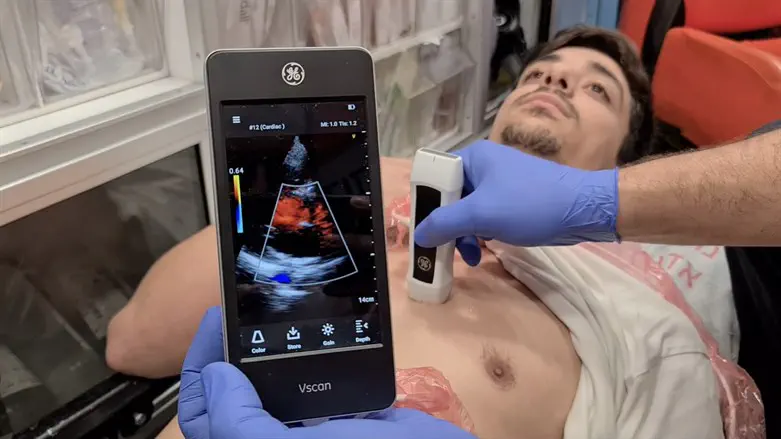
Paramedics with Magen David Adom (MDA), Israel’s national emergency medical service, will soon not only be listening to the hearts of cardiac patients, but literally seeing them too.
Beginning this summer, MDA will be unveiling ultrasound technology aboard its advanced life support Medevac helicopters and its Mobile Intensive Care Unit Ambulances (MICUs).
Initially, the ultrasound will be used primarily to view the hearts of patients in suspected cardiac arrest or deep shock, and to help paramedics establish IV lines in patients with hard-to-detect veins, an important consideration when getting potentially lifesaving medications into patients quickly.
“This is yet another step by Magen David Adom to bring technologies previously only available in [hospital] emergency departments or clinical settings into our MICUs,” said Dr. Refael Strugo, medical director for MDA.
“Being able to actually see a patient’s heart function through an ultrasound probe, rather than merely observe the heart’s electrical impulses through an ECG (electrocardiogram), provides us with a clearer picture of his condition and enables us to make better informed and potentially lifesaving medical decisions,” he said.
The use of the ultrasound equipment is potentially a game-changer in treating a critical cardiac condition known as pseudo PEA (pulseless electrical activity) in which the patient has no palpable pulse, but ultrasound reveals the presence of ventricular contractility, the semblance of a heartbeat.
“In these cases, rather than initiate electric shocks from a defibrillator or provide chest compressions, the protocol would be to administer fluids and adrenaline in order to raise the patient’s blood pressure, to promote more productive beats,” said Dr. Shafir Botner, director of paramedic training for MDA.
“Without the ultrasound equipment,” he added, “it’s nearly impossible to differentiate these cases from patients with true asystole, where the patient has truly flat-lined and where our response would be different.”
Recent studies have indicated that pseudo PEA, where there’s no palpable pulse, but actual heartbeats are occurring, is far more common than previously thought, an indication many patients would benefit from having the ultrasound aboard MDA’s advanced life support vehicles.
Several hundred of MDA’s more than 1,000 paramedics, the most highly trained of the three grades of emergency medical technicians at MDA, have already been trained to use the new equipment. The rest of MDA’s paramedics will be fully trained by the end of this year.
MDA will also use the ultrasound technology to quickly find veins in patients to establish IV lines, a critical capability when paramedics need to administer lifesaving medications.
“Even in patients where good veins are hard to find, we can see veins very clearly with the ultrasound,” Dr. Botner said.
With additional training in the future, he added, MDA paramedics will eventually also be using the ultrasound to detect other conditions, such as tension pneumothorax, in which the patient’s lungs leech air into the chest cavity, a potentially fatal condition that can prevent the patient from breathing.
“The ultrasound is a versatile tool that our paramedics can use to diagnose a number of conditions and ultimately save even more lives,” Dr. Strugo said.
