The prevalence of dental developmental anomalies (DDA) in survivors of childhood cancer differ according to the type of cancer treatment administered, according to researchers at the Hebrew University (HU)-Hadassah School of Dental Medicine.
In a new study published in Nature, researchers assessed the prevalence of DDA among childhood cancer survivors according to types of treatment ─ chemotherapy, radiotherapy, or surgery as well as disease type and age during treatment. They found that combined chemotherapy and radiotherapy ─ particularly radiation to the head and neck area ─ indicated an increased DDA risk. According to the study, the first signs of dental disturbances can be expected within one or two years of the anticancer treatment.
“Childhood cancer treatment is a success story of modern medicine,” shared HU’s Dr. Elinor Halperson. “Effective treatments are now available for previously untreatable diseases. However, children seem to be particularly vulnerable to the harmful effects of radiotherapy and chemotherapy. This growing population of child and young adult cancer survivors require considerable attention from the medical and dental community as we identify future risks.”
The HU study population consisted of 121 individuals who received general annual examinations during 2017–2019, including full oro-dental examinations. Researchers examined the records of patients who received anticancer treatment at HU-Hadassah’s Department of Pediatric Hematology–Oncology before age 18.
DDA was observed in nearly half the individuals (46%), in 9% of teeth. Anomalies were prevalent in 43% of those children who received chemotherapy without radiation, in 52% who also received radiotherapy, and in 60% of those who received head and neck radiotherapy. Patients who received only chemotherapy at six years or younger had a higher number of malformed teeth. No specific chemotherapy agent was found to be associated with a higher risk for dental side effects.
Abnormalities included missing or small teeth, root development and enamel structure damage, over-retention of primary teeth; impaction; premature eruption; decreased temporomandibular joint (TMJ) mobility; inability to open the mouth or jaw, and facial deformities.
The most significant differences between boys and girls’ dental anomalies were a higher incidence of microdontia among females and a greater prevalence for decayed teeth among males.
"This highlights the importance of dental care for individuals who received oncology treatment up to age six, particularly if it was combined with radiotherapy in the head or the neck region," Halperson explained. "This kind of cross-sectional examination can be enhanced in large medical centers to identify the risks of adverse dental effects for specific treatments at particular stages of child development, and to establish international guidelines for follow-up and treatment."
The research team includes Dr. Vered Matalon, Dr. Karin Herzog, Dr. Avia Fux-Noy, Dr. Aviv Shmueli, Prof. Diana Ram, and Prof. Moti Moskovitz of the HU Faculty of Dental Medicine, Department of Pediatric Dentistry, Hadassah Medical Center, and Dr. Gal Goldstein and Dr. Shirly Saieg Spilberg of HU’s Faculty of Medicine, Department of Pediatric Hematology.
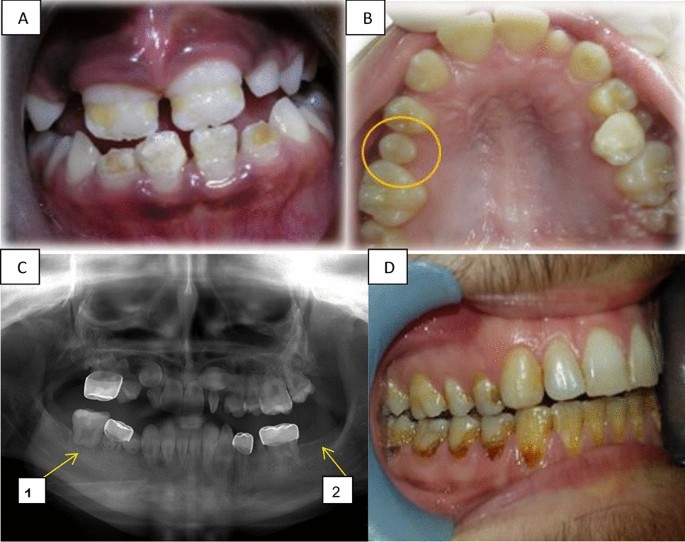
Long term dental effects. (A) Hypoplasia in the front upper and lower teeth of a girl aged 9 years, treated for ALL at age 3.5 years. (B) Microdontia showing the second upper right premolar in a girl of12 years, treated for neuroblastoma at age 4 years. (C) A panoramic radiograph of a 12-year-old boy diagnosed with Burkitt's lymphoma at age 4 years, revealing: C1. Altered root development at the first lower right molar, C2. Hypodontia of the second lower left molar. (D) Radiation caries in a 21-year-old boy treated for neuroectodermal tumor at age 14 years. CREDIT: Elinor Halperson/Hebrew University-Hadassah School of Dental Medicine.
